Evaluation of inflammatory markers in pregnancies with hyperemesis gravidarum
Inflammatory markers in pregnancies with hyperemesis gravidarum
Keywords:
Hyperemesis gravidarum, procalcitonin, neutrophil-lymphocyte ratio, platelet-lymphocyte ratioAbstract
Background/Aim: Hyperemesis gravidarum (HG) is a severe clinical condition characterized by intractable nausea and vomiting during pregnancy, yet its exact etiology remains elusive. This study aimed to investigate the association between HG and the inflammatory markers procalcitonin (PCT), neutrophil-to-lymphocyte ratio (NLR), and platelet-to-lymphocyte ratio (PLR) to better understand the role of systemic inflammation in the disorder.
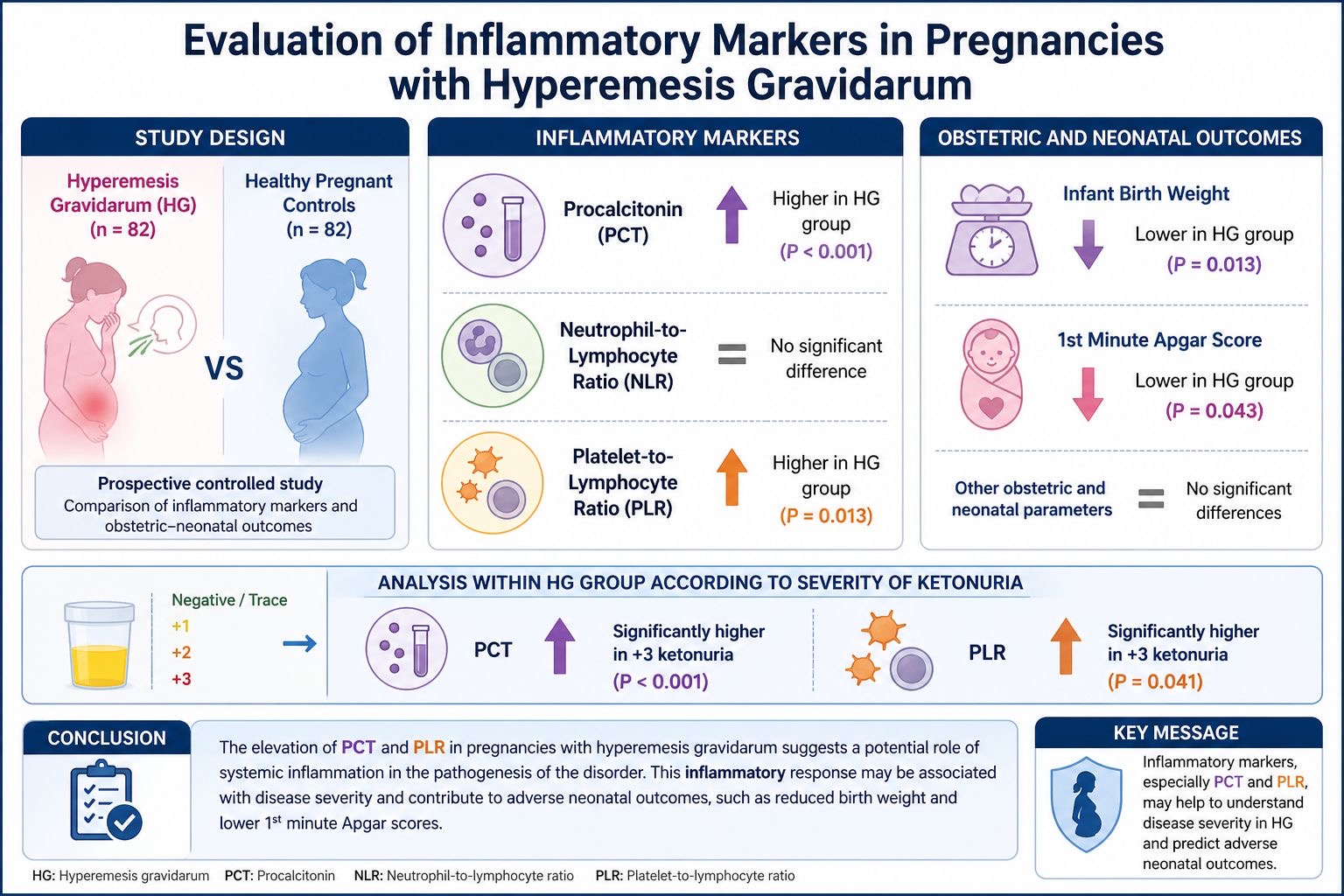
Methods: This prospective controlled study included 82 pregnant women diagnosed with HG and 82 healthy pregnant controls. Demographic data, serum PCT levels, NLR, PLR, and obstetric and neonatal outcomes were compared between the two groups. Additionally, patients in the HG group were analyzed according to the severity of ketonuria.
Results: No significant differences were observed in demographic characteristics between the groups. The HG group demonstrated significantly higher PCT and PLR levels than the control group (P<0.001 and P=0.013, respectively). Regarding obstetric and neonatal outcomes, both infant birth weight and first-minute Apgar scores were significantly lower in the HG group (P=0.013 and P=0.043, respectively). Within the HG group, patients exhibiting +3 urinary ketones had significantly higher PCT and PLR values compared to those with lower ketone levels (P<0.001 and P=0.041, respectively). No significant differences were found in other obstetric and neonatal parameters.
Conclusion: The elevation of PCT and PLR in pregnant women with HG suggests a potential involvement of systemic inflammation in the pathogenesis of the disorder. This inflammatory response may be associated with disease severity and contribute to adverse neonatal outcomes, such as reduced birth weight and lower first-minute Apgar scores.
Downloads
References
Lacasse A, Rey E, Ferreira E, Morin C, Bérard A. Nausea and vomiting of pregnancy: what about quality of life? BJOG. 2008;115(12):1484-93. DOI: https://doi.org/10.1111/j.1471-0528.2008.01891.x
Godsey RK, Newman RB. Hyperemesis gravidarum. A comparison of single and multiple admissions. J Reprod Med. 1991;36(4):287-90.
Brzana RJ, Koch KL. Gastroesophageal reflux disease presenting with intractable nausea. Ann Intern Med. 1997;126(9):704-7. DOI: https://doi.org/10.7326/0003-4819-126-9-199705010-00005
Eliakim R, Abulafia O, Sherer DM. Hyperemesis gravidarum: a current review. Am J Perinatol. 2000;17(4):207-18. DOI: https://doi.org/10.1055/s-2000-9424
Netravathi M, Sinha S, Taly AB, Bindu PS, Bharath RD. Hyperemesis-gravidarum-induced Wernicke's encephalopathy: serial clinical, electrophysiological and MR imaging observations. J Neurol Sci. 2009;284(1-2):214-6. DOI: https://doi.org/10.1016/j.jns.2009.05.004
Bailit JL. Hyperemesis gravidarium: Epidemiologic findings from a large cohort. Am J Obstet Gynecol. 2005;193(3 Pt 1):811-4. DOI: https://doi.org/10.1016/j.ajog.2005.02.132
Veenendaal MV, van Abeelen AF, Painter RC, van der Post JA, Roseboom TJ. Consequences of hyperemesis gravidarum for offspring: a systematic review and meta-analysis. BJOG. 2011;118(11):1302-13. DOI: https://doi.org/10.1111/j.1471-0528.2011.03023.x
Liu C, Zhao G, Qiao D, Wang L, He Y, Zhao M, et al. Emerging Progress in Nausea and Vomiting of Pregnancy and Hyperemesis Gravidarum: Challenges and Opportunities. Front Med (Lausanne). 2022;8:809270. doi: 10.3389/fmed.2021.809270. DOI: https://doi.org/10.3389/fmed.2021.809270
Kurt RK, Güler A, Silfeler DB, Ozçil MD, Karateke A, Hakverdi AU, et al. Relation of inflammatory markers with both presence and severity of hyperemesis gravidarum. Ginekol Pol. 2014;85(8):589-93. DOI: https://doi.org/10.17772/gp/1776
Caglayan EK, Engin-Ustun Y, Gocmen AY, Sarı N, Seckin L, Kara M, et al. Is there any relationship between serum sirtuin-1 level and neutrophil-lymphocyte ratio in hyperemesis gravidarum? J Perinat Med. 2016;44(3):315-20. DOI: https://doi.org/10.1515/jpm-2015-0178
Niemeijer MN, Grooten IJ, Vos N, Bais JM, van der Post JA, Mol BW, et al. Diagnostic markers for hyperemesis gravidarum: A systematic review and meta-analysis. Am J Obstet Gynecol. 2014;211(2):150.e1-15. DOI: https://doi.org/10.1016/j.ajog.2014.02.012
Hacımustafaoğlu M. Procalcitonin as an Acute Phase Reactant. J Pediatr Inf. 2017;11(4):196-7. DOI: https://doi.org/10.5578/ced.201752
Wei JX, Verity A, Garle M, Mahajan R, Wilson V. Examination of the effect of procalcitonin on human leucocytes and the porcine isolated coronary artery. Br J Anaesth. 2008;100(5):612-21. DOI: https://doi.org/10.1093/bja/aen073
Gogos CA, Drosou E, Bassaris HP, Skoutelis A. Pro- versus anti-inflammatory cytokine profile in patients with severe sepsis: a marker for prognosis and future therapeutic options. J Infect Dis. 2000;181(1):176-80. DOI: https://doi.org/10.1086/315214
Kafkas N, Venetsanou K, Patsilinakos S, Voudris V, Antonatos D, Kelesidis K, et al. Procalcitonin in acute myocardial infarction. Acute Card Care. 2008;10(1):30-6. DOI: https://doi.org/10.1080/17482940701534800
Sapmaz E, Bulut V, Çelik A, Akbulut H, İlhan F, Hanay F. Preeklampsi Vakalarında Nötrofil, İnterlökin-8 ve Prokalsitonin Düzeylerinin İncelenmesi. J Clin Obstet Gynecol. 2006;16(4):119-23.
Torbé A. Maternal plasma procalcitonin concentrations in pregnancy complicated by preterm premature rupture of membranes. Mediators Inflamm. 2007;2007:35782. doi: 10.1155/2007/35782. DOI: https://doi.org/10.1155/2007/35782
Kirbas A, Biberoglu E, Daglar K, İskender C, Erkaya S, Dede H, et al. Neutrophil-to-lymphocyte ratio as a diagnostic marker of intrahepatic cholestasis of pregnancy. Eur J Obstet Gynecol Reprod Biol. 2014;180:12-5. DOI: https://doi.org/10.1016/j.ejogrb.2014.05.042
Sargın MA, Yassa M, Taymur BD, Celik A, Ergun E, Tug N. Neutrophil-to-lymphocyte and platelet-to-lymphocyte ratios: are they useful for predicting gestational diabetes mellitus during pregnancy? Ther Clin Risk Manag. 2016;12:657-65. DOI: https://doi.org/10.2147/TCRM.S104247
Çintesun E, Akar S, Gul A, Çintesun FNI, Sahin G, Ezveci H, et al. Subclinical inflammation markers in hyperemesis gravidarum and ketonuria: A case-control study. J Lab Physicians. 2019;11(2):149-53. DOI: https://doi.org/10.4103/JLP.JLP_151_18
Ethier JL, Desautels DN, Templeton AJ, Oza A, Amir E, Lheureux S. Is the neutrophil-to-lymphocyte ratio prognostic of survival outcomes in gynecologic cancers? A systematic review and meta-analysis. Gynecol Oncol. 2017;145(3):584-94. DOI: https://doi.org/10.1016/j.ygyno.2017.02.026
Verit FF, Cetin O, Yildirim O, Keskin S, Yucel O, Yalcinkaya S. Neutrophil to lymphocyte ratio is superior to platelet to lymphocyte ratio as an early predictor of moderate/severe ovarian hyperstimulation syndrome. J Obstet Gynaecol. 2017;37(5):639-43. DOI: https://doi.org/10.3109/01443615.2014.920792
Serin S, Avcı F, Ercan O, Köstü B, Bakacak M, Kıran H. Is neutrophil/lymphocyte ratio a useful marker to predict the severity of pre-eclampsia? Pregnancy Hypertens. 2016;6(1):22-5. DOI: https://doi.org/10.1016/j.preghy.2016.01.005
McCarthy FP, Lutomski JE, Greene RA. Hyperemesis gravidarum: current perspectives. Int J Womens Health. 2014;6:719-25. DOI: https://doi.org/10.2147/IJWH.S37685
Soysal C, Işıkalan MM, Bıyık İ, Erten Ö, İnce O. The relationship between inflammation markers and ketonuria in hyperemesis gravidarum. J Obstet Gynaecol Res. 2021;47(9):3078-83. doi: 10.1111/jog.14857. DOI: https://doi.org/10.1111/jog.14857
Kan E, Emektar E, Corbacioglu K, Safak T, Sariaydin T, Cevik Y. Evaluation of relationship between inflammatory markers and hyperemesis gravidarum in patients admitted to emergency department. Am J Emerg Med. 2020;38(2):292-5. DOI: https://doi.org/10.1016/j.ajem.2019.05.007
London V, Grube S, Sherer DM, Abulafia O. Hyperemesis Gravidarum: A Review of Recent Literature. Pharmacology. 2017;100(3-4):161-71. doi: 10.1159/000477853. DOI: https://doi.org/10.1159/000477853
Uçkan K, Demir H, Demir C. Maternal serum ischemia-modified albumin (IMA), total-sulphydryl concentrations, and some subclinic inflammatory markers in hyperemesis gravidarum (HG). Taiwan J Obstet Gynecol. 2023;62(1):101-6. DOI: https://doi.org/10.1016/j.tjog.2022.10.006
Engin-Ustun Y, Tonguç E, Var T, Deveer R, Yilmaz R, Danisman N, et al. Vaspin and C-reactive protein levels in hyperemesis gravidarum. Eur Rev Med Pharmacol Sci. 2013;17(1):138-40.
Mangogna A, Agostinis C, Ricci G, Romano F, Bulla R. Overview of procalcitonin in pregnancy and in pre-eclampsia. Clin Exp Immunol. 2019;198(1):37-46. DOI: https://doi.org/10.1111/cei.13311
Beyazit F, Öztürk FH, Pek E, Ünsal MA. Evaluation of the hematologic system as a marker of subclinical inflammation in hyperemesis gravidarum. Ginekol Pol. 2017;88(6):315-9. DOI: https://doi.org/10.5603/GP.a2017.0059
Yao C, Liu X, Tang Z. Prognostic role of neutrophil-lymphocyte ratio and platelet-lymphocyte ratio for hospital mortality in patients with AECOPD. Int J Chron Obstruct Pulmon Dis. 2017;12:2285-90. DOI: https://doi.org/10.2147/COPD.S141760
Lee SK, Lee SC, Park JW, Kim SJ. The utility of the preoperative neutrophil-to-lymphocyte ratio in predicting severe cholecystitis: a retrospective cohort study. BMC Surg. 2014;14:100. DOI: https://doi.org/10.1186/1471-2482-14-100
Haram A, Boland MR, Kelly ME, Bolger JC, Waldron RM, Kerin MJ. The prognostic value of neutrophil-to-lymphocyte ratio in colorectal cancer: A systematic review. J Surg Oncol. 2017;115(4):470-9. DOI: https://doi.org/10.1002/jso.24523
Seropian IM, Romeo FJ, Pizarro R, Vulcano NO, Posatini RA, Marenchino RG, et al. Neutrophil-to-lymphocyte ratio and platelet-to-lymphocyte ratio as predictors of survival after heart transplantation. ESC Heart Fail. 2018;5(1):149-56. DOI: https://doi.org/10.1002/ehf2.12199
Ilhan G, Atmaca FFV, Altan E, Zebitay AG, Sozen H, Akyol H, et al. Evaluation of Neutrophil-Lymphocyte Ratio, Platelet-Lymphocyte Ratio and2 Red Blood Cell Distribution Width-Platelet Ratio for Diagnosis of Premature Ovarian Insufficiency. J Family Reprod Health. 2016;10(4):211-6.
Tokmak A, Yildirim G, Öztaş E, Akar S, Erkenekli K, Gülşen P, et al. Use of Neutrophil-to-Lymphocyte Ratio Combined With CA-125 to Distinguish Endometriomas From Other Benign Ovarian Cysts. Reprod Sci. 2016;23(6):795-802. DOI: https://doi.org/10.1177/1933719115620494
Tayfur C, Burcu DC, Gulten O, Dundar B, Guclu T, Ozdenoglu O, et al. Association between platelet to lymphocyte ratio, plateletcrit and the presence and severity of hyperemesis gravidarum. J Obstet Gynaecol Res. 2017;43(3):498-504. DOI: https://doi.org/10.1111/jog.13228
Downloads
- 121 185
Published
Issue
Section
How to Cite
License
Copyright (c) 2026 Zehra Dilara Arslan, Aysun Tekeli̇ Taşkömür
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.















