Stroke after coronary artery bypass grafting (CABG): A single center experience
Stroke incidence after CABG surgery
Keywords:
Stroke, Hypertension, Diabetes, Hyperlipidemia, Risk factors., coronary artery bypass graftingAbstract
Background/Aim: Coronary artery bypass grafting (CABG) is among the ten most commonly performed surgical procedures in the United States. Despite advances in surgical techniques and perioperative care, stroke remains a serious complication, associated with significant morbidity and mortality. The aim of this study is to determine the incidence of stroke following CABG at a single institution, compare it with published rates from other centers, and identify common perioperative risk factors to support targeted, population specific prevention strategies.
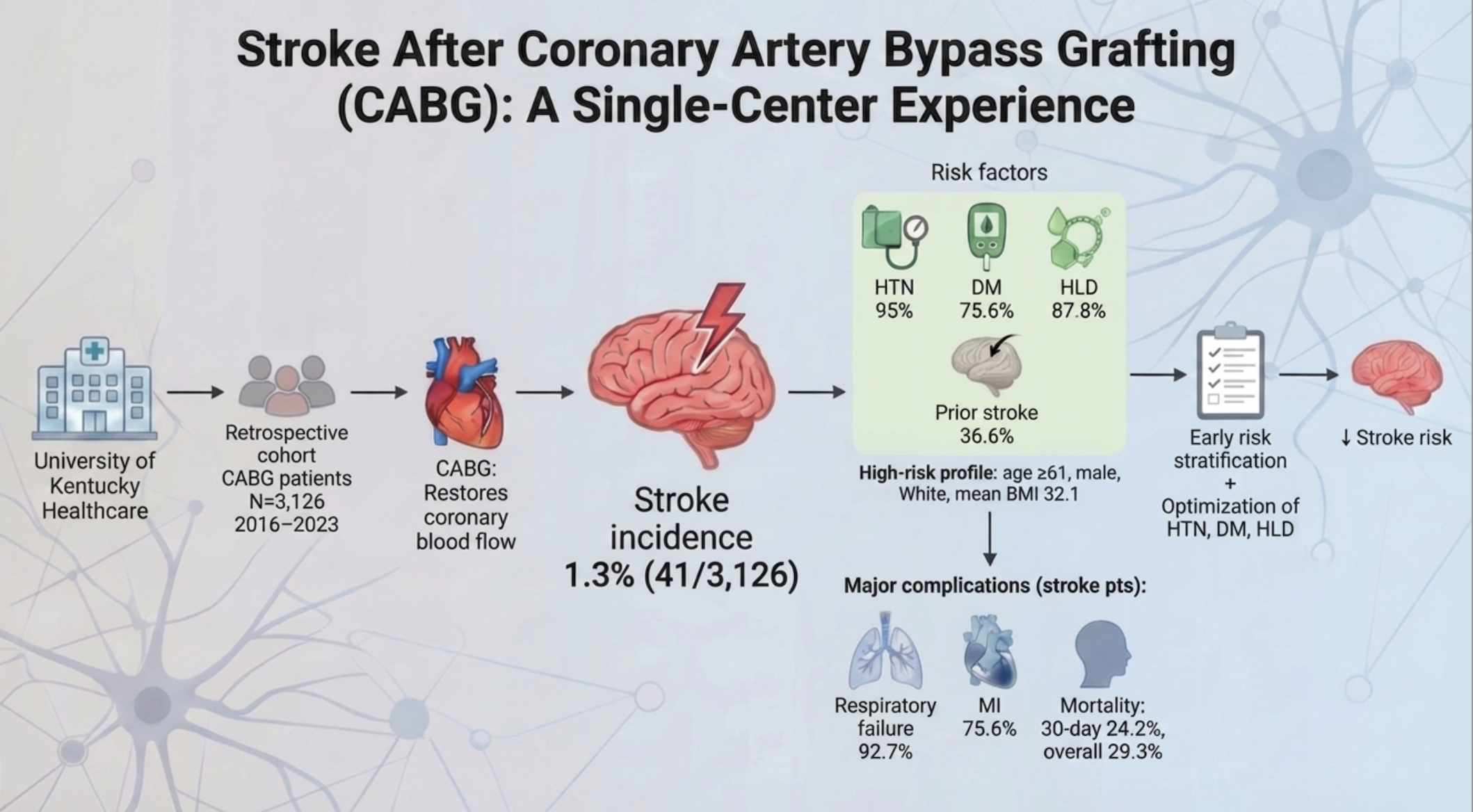
Methods: We conducted a retrospective chart review of 3,126 adult patients who underwent isolated coronary artery bypass grafting at our institution between 2016 and 2023. Data were collected on demographic variables, comorbidities, and perioperative factors. The incidence of postoperative stroke was determined, and comparative statistical analysis were performed to identify potential risk factors.
Results: Postoperative stroke occurred in 1.3% of patients (41 of 3,126). The majority of affected individuals were white males aged 61 years or older. Common preoperative comorbidities included hypertension (95%), hyperlipidemia (87.8%), diabetes mellitus (75.6%), and a history of atrial fibrillation (26.7%). Postoperative respiratory failure was observed in 92.7% of stroke patients. Overall mortality in this group was 29.3%, with 24.2% of the casualties occurring within 30 days of surgery and an additional 4.9% within five years.
Conclusions: The incidence of stroke following CABG at our institution (1.3%) falls within the range reported in the literature (1.2%–5.2%). Stroke was associated with longer hospital stays and increased mortality. Hypertension, diabetes mellitus, and hyperlipidemia emerged as the most prominent risk factors. These findings highlight the need for early risk stratification and proactive management of modifiable comorbidities to minimize stroke incidence in patients undergoing CABG.
Downloads
References
Lorusso R, Moscarelli M, Di Franco A, Grazioli V, Nicolini F, Gherli T, et al. Association between coronary artery bypass surgical techniques and postoperative stroke. J Am Heart Assoc. 2019;8:e013650. doi:10.1161/JAHA.119.013650. DOI: https://doi.org/10.1161/JAHA.119.013650
Laimoud M, Maghirang M, Alanazi M, Al-Mutlaq SM, Althibait SA, Alanazi B, et al. Predictors and clinical outcomes of post-coronary artery bypass grafting cerebrovascular strokes. Egypt Heart J. 2022;74:76. Erratum in: Egypt Heart J. 2022;74:79. doi:10.1186/s43044-022-00315-4. DOI: https://doi.org/10.1186/s43044-022-00315-4
Mohamed MO, Hirji S, Mohamed W, Percy E, Braidley P, Chung J, et al. Incidence and predictors of postoperative ischemic stroke after coronary artery bypass grafting. Int J Clin Pract. 2021;75:e14067. doi:10.1111/ijcp.14067. DOI: https://doi.org/10.1111/ijcp.14067
Jonsson K, Barbu M, Nielsen SJ, Hafsteinsdottir B, Gudbjartsson T, Jensen EM, et al. Perioperative stroke and survival in coronary artery bypass grafting patients: a SWEDEHEART study. Eur J Cardiothorac Surg. 2022;62:ezac025. doi:10.1093/ejcts/ezac025. DOI: https://doi.org/10.1093/ejcts/ezac025
Kroeze VJ, Olsthoorn JR, van Straten AHM, Princee A, Soliman-Hamad MA. Predictors and outcomes of stroke after isolated coronary artery bypass grafting: a single-center experience in 20,582 patients. J Cardiothorac Vasc Anesth. 2023;37:1397–402. doi:10.1053/j.jvca.2023.04.012. DOI: https://doi.org/10.1053/j.jvca.2023.04.012
Shah SMA, Rehman MU, Awan NI, Jan A. To determine the frequency of stroke and common factors leading to it after coronary artery bypass grafting. Pak J Med Sci. 2021;37:261–6. doi:10.12669/pjms.37.1.3242. DOI: https://doi.org/10.12669/pjms.37.1.3242
Jawitz OK, Gulack BC, Brennan JM, Thibault DP, Wang A, O'Brien SM, et al. Association of postoperative complications and outcomes following coronary artery bypass grafting. Am Heart J. 2020;222:220–8. doi:10.1016/j.ahj.2020.02.002. DOI: https://doi.org/10.1016/j.ahj.2020.02.002
Wagner BD, Grunwald GK, Almassi GH, Grover FL, Shroyer ALW. Factors associated with long-term survival in patients with stroke after coronary artery bypass grafting. J Int Med Res. 2020;48:300060520920428. doi:10.1177/0300060520920428. DOI: https://doi.org/10.1177/0300060520920428
Irqsusi M, Schenk Zu Schweinsberg T, Johnson FA, Dielmann K, Ramzan R, Vogt S, et al. Prediction of stroke reconvalescence after coronary bypass surgery indicated by CT scan parameters. J Card Surg. 2022;37:3133–47. doi:10.1111/jocs.16797. DOI: https://doi.org/10.1111/jocs.16797
Mao Z, Zhong X, Yin J, Zhao Z, Hu X, Hackett ML. Predictors associated with stroke after coronary artery bypass grafting: a systematic review. J Neurol Sci. 2015;357:1–7. doi:10.1016/j.jns.2015.07.006. DOI: https://doi.org/10.1016/j.jns.2015.07.006
Roy P, Brahme I, Reddy RP, Wechsler L, Gleason T, Thirumala PD. Meta-analysis of perioperative stroke and mortality in CABG patients with carotid stenosis. Neurologist. 2020;25:113–6. doi:10.1097/NRL.0000000000000277. DOI: https://doi.org/10.1097/NRL.0000000000000277
Gaudino M, Angiolillo DJ, Di Franco A, Capodanno D, Bakaeen F, Farkouh ME, et al. Stroke after coronary artery bypass grafting and percutaneous coronary intervention: incidence, pathogenesis, and outcomes. J Am Heart Assoc. 2019;8:e013032. doi:10.1161/JAHA.119.013032. DOI: https://doi.org/10.1161/JAHA.119.013032
Zhang RJ, Yu XY, Wang J, Lv J, Yu MH, Wang L, et al. Comparison of in-hospital outcomes after coronary artery bypass graft surgery in elders and younger patients: a multicenter retrospective study. J Cardiothorac Surg. 2023;18:53. doi:10.1186/s13019-023-02163-y. DOI: https://doi.org/10.1186/s13019-023-02163-y
Patel BM, Reinert NJ, Al-Robaidi K, Gao X, Fabio A, Esper SA, et al. Independent predictors of perioperative stroke-related mortality after cardiac surgery. J Stroke Cerebrovasc Dis. 2020;29:104711. doi:10.1016/j.jstrokecerebrovasdis.2020.104711. DOI: https://doi.org/10.1016/j.jstrokecerebrovasdis.2020.104711
Bryce Robinson N, Naik A, Rahouma M, Morsi M, Wright D, Hameed I, et al. Sex differences in outcomes following coronary artery bypass grafting: a meta-analysis. Interact Cardiovasc Thorac Surg. 2021;33:841–7. doi:10.1093/icvts/ivab191. DOI: https://doi.org/10.1093/icvts/ivab191
Taha A, Nielsen SJ, Franzén S, Rezk M, Ahlsson A, Friberg L, et al. Stroke risk stratification in patients with postoperative atrial fibrillation after coronary artery bypass grafting. J Am Heart Assoc. 2022;11:e024703. doi:10.1161/JAHA.121.024703. DOI: https://doi.org/10.1161/JAHA.121.024703
Benedetto U, Gaudino MF, Dimagli A, Gerry S, Gray A, Lees B, et al. Postoperative atrial fibrillation and long-term risk of stroke after isolated coronary artery bypass graft surgery. Circulation. 2020;142:1320–9. doi:10.1161/CIRCULATIONAHA.120.046940. DOI: https://doi.org/10.1161/CIRCULATIONAHA.120.046940
Amundson B, Hormes J, Katema A, Rathakrishnan P, Edwards JK, Esper G, et al. Timing of recognition for perioperative strokes following cardiac surgery. J Stroke Cerebrovasc Dis. 2020;29:105336. doi:10.1016/j.jstrokecerebrovasdis.2020.105336. DOI: https://doi.org/10.1016/j.jstrokecerebrovasdis.2020.105336
Paquin A, Poirier P, Beaudoin J, Piché ME. Secondary prevention after CABG: do new agents change the paradigm? Curr Opin Cardiol. 2020;35(6):664–72. doi:10.1097/HCO.0000000000000783. DOI: https://doi.org/10.1097/HCO.0000000000000783
Downloads
- 234 392
Published
Issue
Section
How to Cite
License
Copyright (c) 2026 Roxana Ponce Parrado, Sibu Saha
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.















